Author Archives: Dr. Vaidya Karanvir Singh
How Ayurvedic Treatment is Best for Treating PCOD
- April 3, 2025
- Posted by Dr. Vaidya Karanvir Singh
- 0 Comment(s)
Polycystic Ovarian Disease (PCOD) is a common hormonal disorder that affects many women of reproductive age. It leads to irregular menstrual cycles, weight gain, excessive hair growth, and infertility. While modern medicine offers treatments like hormonal therapy and medications, Ayurveda provides a natural and holistic approach to managing PCOD by addressing its root cause rather than just the symptoms.
Understanding PCOD in Ayurveda
According to Ayurveda, PCOD is primarily caused by an imbalance in the three doshas—Vata, Pitta, and Kapha. The main culprit is an aggravated Kapha dosha, which disrupts metabolism and leads to the formation of cysts in the ovaries. Ayurveda focuses on detoxifying the body, balancing hormones naturally, and improving overall reproductive health.
Ayurvedic Treatments for PCOD
1. Herbal Remedies
Several Ayurvedic herbs help in managing PCOD effectively:
- Ashwagandha (Withania somnifera): Helps reduce stress and balances hormones.
- Shatavari (Asparagus racemosus): Supports ovarian health and regulates menstrual cycles.
- Guduchi (Tinospora cordifolia): Enhances immunity and detoxifies the body.
- Cinnamon (Dalchini): Improves insulin sensitivity and helps with weight management.
- Turmeric (Haldi): Has anti-inflammatory properties that reduce cyst formation.
2. Panchakarma Therapy
Detoxification through Panchakarma helps remove toxins and balance doshas. The most effective Panchakarma therapies for PCOD include:
- Vamana (Therapeutic Emesis): Eliminates excess Kapha dosha.
- Virechana (Purgation Therapy): Detoxifies the liver and improves digestion.
- Basti (Medicated Enema): Regulates hormonal imbalance and improves reproductive health.
3. Dietary and Lifestyle Modifications
Ayurveda emphasizes a proper diet and lifestyle to manage PCOD effectively.
- Diet Recommendations:
- Eat warm, fresh, and easily digestible foods.
- Include whole grains, green leafy vegetables, fruits, nuts, and seeds.
- Avoid processed foods, dairy, excess sugar, and fried foods.
- Drink herbal teas like fenugreek, ginger, and tulsi tea.
- Exercise and Yoga:
- Practicing yoga asanas like Surya Namaskar, Bhujangasana, and Baddha Konasana helps improve ovarian function.
- Regular physical activity such as walking, swimming, and meditation helps manage stress and insulin resistance.
Why Ayurveda is the Best Approach for PCOD
- Addresses Root Cause: Ayurveda focuses on treating the underlying hormonal imbalance instead of just managing symptoms.
- No Side Effects: Ayurvedic medicines are natural and do not cause harmful side effects like hormonal pills.
- Improves Overall Health: Ayurveda not only treats PCOD but also enhances overall well-being by balancing the body, mind, and spirit.
- Long-term Relief: Unlike allopathic treatments, which offer temporary solutions, Ayurveda provides sustainable healing through natural therapies.
Conclusion
Ayurvedic treatment for PCOD is highly effective as it adopts a holistic approach by combining herbal remedies, Panchakarma therapies, dietary changes, and yoga. This natural way of healing provides long-term benefits without any adverse side effects, making Ayurveda the best choice for managing and curing PCOD.
What is Parkinson disease? How it can be treated by ayurvedic remedies
- March 25, 2025
- Posted by Dr. Vaidya Karanvir Singh
- 0 Comment(s)
What is Parkinson’s Disease?
Parkinson’s Disease (PD) is a progressive neurological disorder that affects movement. It is caused by the degeneration of dopamine-producing neurons in the brain, particularly in the substantia nigra region. Dopamine is a neurotransmitter responsible for smooth and coordinated muscle movements. As its levels decrease, patients experience motor and non-motor symptoms.
Symptoms of Parkinson’s Disease
Motor Symptoms:
Tremors (shaking of hands, legs, jaw, or face)
Muscle rigidity (stiffness in limbs and trunk)
Bradykinesia (slowness of movement)
Postural instability (balance and coordination problems)
Non-Motor Symptoms:
Cognitive decline and memory problems
Sleep disturbances
Depression and anxiety
Digestive issues like constipation
Loss of sense of smell
Causes and Risk Factors
Aging and oxidative stress
Genetic predisposition
Exposure to toxins and pesticides
Chronic stress and unhealthy lifestyle
Ayurvedic Perspective on Parkinson’s Disease
In Ayurveda, Parkinson’s Disease is correlated with “Kampavata”, a disorder caused by an imbalance of Vata dosha (which governs movement and nervous functions). Excessive Vata can lead to degeneration of brain tissues, resulting in tremors and muscle stiffness. Ayurveda aims to balance Vata, strengthen the nervous system, and improve overall health.
Ayurvedic Remedies for Parkinson’s Disease
1. Ayurvedic Herbs for Parkinson’s Disease
Mucuna Pruriens (Kaunch Beej): A natural source of L-Dopa, the precursor to dopamine, which helps improve motor function.
Brahmi (Bacopa Monnieri): Enhances brain function, memory, and nerve regeneration.
Ashwagandha (Withania Somnifera): Reduces stress, strengthens nerves, and improves muscle coordination.
Shankhpushpi (Convolvulus Pluricaulis): Supports cognitive function and helps in reducing tremors.
Guduchi (Tinospora Cordifolia): Acts as a neuroprotective agent and enhances immunity.
Turmeric (Curcuma Longa): Contains curcumin, which reduces inflammation and oxidative stress in the brain.
2. Ayurvedic Formulations for Parkinson’s Disease
Vata-Pacifying Oils: Abhyanga (body massage) with Mahanarayan Oil, Bala Taila, or Dashmool Oil helps reduce muscle stiffness and tremors.
Medhya Rasayana (Brain Tonics): Ayurvedic formulations like Saraswatarishta and Brahmi Ghrita improve cognitive function.
Ashwagandha Churna: Taken with milk, it strengthens the nervous system and reduces stress.
Rasayana Therapy: Includes rejuvenating herbs like Shilajit and Chyawanprash to slow down neurodegeneration.
3. Lifestyle and Dietary Recommendations
Dietary Changes:
Include warm, nourishing, and easily digestible foods.
Consume healthy fats like ghee, nuts, and seeds to support brain function.
Avoid processed foods, excess caffeine, and dry foods that aggravate Vata.
Stay hydrated and eat fiber-rich foods to prevent constipation.
Yoga and Meditation:
Yoga Asanas: Vajrasana, Tadasana, and Sukhasana help improve mobility and balance.
Pranayama (Breathing Exercises): Anulom-Vilom and Bhramari Pranayama calm the nervous system.
Meditation: Reduces stress and improves mental clarity.
Daily Routine (Dinacharya):
Regular head and body massage with warm herbal oils.
Sun exposure for vitamin D, which supports nerve function.
Avoid excessive stress and follow a disciplined lifestyle.
Conclusion
Ayurvedic treatment for Parkinson’s Disease focuses on balancing Vata dosha, improving brain function, and slowing disease progression through herbs, dietary changes, yoga, and lifestyle modifications. While Ayurveda cannot completely cure Parkinson’s, it can significantly enhance the quality of life and manage symptoms naturally. Integrating Ayurvedic therapies with conventional medical care can help achieve better results.
What is Benign prostatic hyperplasia (BPH)? How it can be treated by ayurvedic remedies
- March 25, 2025
- Posted by Dr. Vaidya Karanvir Singh
- 0 Comment(s)
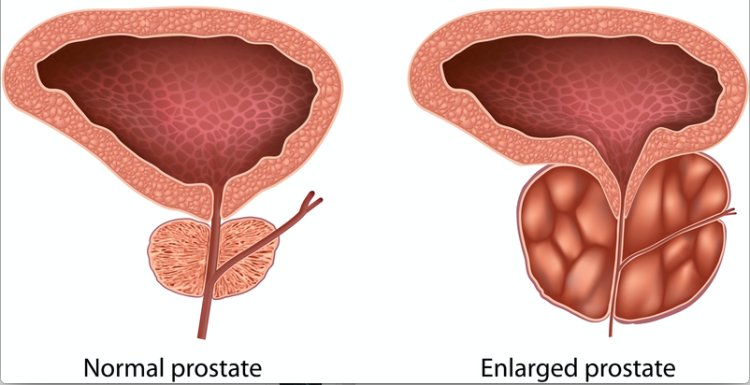
What is Benign Prostatic Hyperplasia (BPH)?
Benign Prostatic Hyperplasia (BPH) is a non-cancerous enlargement of the prostate gland that commonly affects older men. The prostate is a small gland located below the bladder, surrounding the urethra. As the gland enlarges, it can compress the urethra, leading to urinary problems such as:
Frequent urination, especially at night (nocturia)
Difficulty in starting and stopping urination
Weak or interrupted urine flow
Feeling of incomplete bladder emptying
Dribbling at the end of urination
BPH is primarily caused by hormonal changes with aging, particularly an increase in dihydrotestosterone (DHT) levels. Chronic inflammation and poor lifestyle choices may also contribute to the condition.
Ayurvedic Approach to BPH Treatment
Ayurveda focuses on balancing the doshas (Vata, Pitta, and Kapha) and improving urinary function naturally. In BPH, an imbalance of Vata dosha (which controls movement, including urination) is often responsible for the condition. Ayurvedic remedies help in reducing prostate size, improving urine flow, and strengthening the urinary system.
1. Ayurvedic Herbs for BPH
Several Ayurvedic herbs have been traditionally used to treat prostate enlargement:
Varuna (Crataeva nurvala): Helps in reducing prostate swelling and improving urine flow.
Gokshura (Tribulus terrestris): Acts as a diuretic and strengthens the urinary system.
Shatavari (Asparagus racemosus): Supports reproductive health and reduces inflammation.
Kanchnaar (Bauhinia variegata): Helps in reducing glandular swellings, including prostate enlargement.
Pashanbheda (Bergenia ligulata): Prevents urinary infections and aids in smooth urine flow.
Punarnava (Boerhavia diffusa): Acts as a natural diuretic and reduces prostate-related swelling.
2. Ayurvedic Formulations for BPH
Chandraprabha Vati: A classical Ayurvedic medicine used to support prostate health and improve urinary function.
Gokshuradi Guggulu: Helps in reducing inflammation and supports urinary function.
Shilajit Rasayana: Strengthens the reproductive and urinary system.
Kanchnaar Guggulu: Helps in shrinking glandular swellings like BPH.
3. Lifestyle and Dietary Recommendations
Increase fluid intake: Drink warm water with a pinch of turmeric to reduce inflammation.
Include fiber-rich foods: Such as fruits, vegetables, and whole grains to prevent constipation, which can worsen BPH symptoms.
Avoid spicy, oily, and processed foods: These can aggravate Pitta and worsen inflammation.
Regular exercise and yoga: Poses like Vajrasana and Malasana help in improving urinary flow.
Avoid alcohol and caffeine: These can irritate the bladder and increase urinary frequency.
Conclusion
Ayurvedic remedies for BPH focus on herbal treatments, dietary changes, and lifestyle modifications to manage symptoms and improve prostate health. Regular use of Ayurvedic medicines along with a balanced lifestyle can help in naturally reducing prostate enlargement and preventing complications.
What is Ascites? How it can be Treated in Ayurveda?
- March 4, 2025
- Posted by Dr. Vaidya Karanvir Singh
- 0 Comment(s)
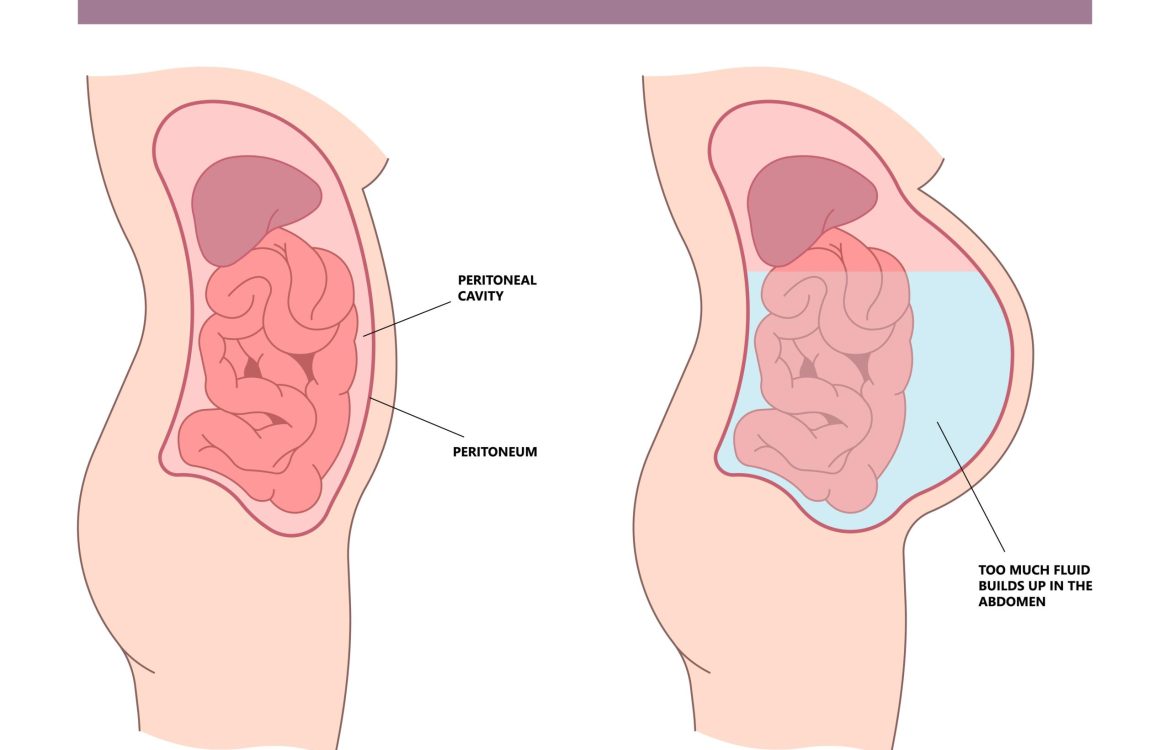
In Ayurveda, Ascites (Jalodara) is considered a subtype of Udara Roga (Abdominal Disorders) and is primarily caused by an imbalance of Vata and Kapha Dosha along with Agni Dushti (Digestive Fire Impairment). The main causes include:
• Liver disorders (cirrhosis, hepatitis)
• Kidney dysfunction
• Heart diseases
• Obstruction in channels (Srotorodha) leading to fluid accumulation
• Ama (Toxins) accumulation in the abdomen
• Excessive alcohol consumption
Ayurveda focuses on eliminating the root cause by balancing Doshas, improving digestion, and detoxifying the body through herbal medicines, Panchakarma therapies, and dietary regulations.
Types of Ascites in Modern Science
Modern medicine classifies Ascites based on its causative factors and severity:
1. Transudative Ascites: Caused by increased pressure in the portal vein due to liver cirrhosis, heart failure, or kidney disease.
2. Exudative Ascites: Due to infection, inflammation, or malignancies (e.g., tuberculosis, cancer, pancreatitis).
3. Malignant Ascites: Caused by cancerous tumors (e.g., ovarian, liver, or pancreatic cancer).
4. Chylous Ascites: Due to lymphatic obstruction, leading to a milky fluid accumulation.
5. Hemorrhagic Ascites: Caused by ruptured blood vessels or trauma, leading to blood in the peritoneal cavity.
Difference Between Ayurvedic and Modern Management of Ascites
Aspect Ayurveda Modern Medicine
Approach Focuses on root cause healing, balancing Doshas, and detoxifying the liver and kidneys. Treats symptoms using diuretics, paracentesis (fluid removal), and liver transplant in severe cases.
Treatment Focus Strengthens digestive fire (Agni), eliminates toxins, and corrects metabolism. Focuses on fluid removal and symptomatic relief but may not address the root cause.
Use of Chemicals Uses natural herbs, Panchakarma therapies, and diet-based management. Involves synthetic drugs, diuretics, and invasive procedures.
Long-Term Benefits Prevents recurrence by correcting metabolic imbalances and improving digestion. Provides temporary relief; fluid accumulation often recurs.
Common Ayurvedic Protocol for Healing Ascites from Root Cause
1. Panchakarma (Detoxification Therapies)
• Virechana (Purgation Therapy): Removes excess Pitta toxins from the liver.
• Basti (Medicated Enema): Corrects Vata imbalance and improves kidney function.
• Raktamokshana (Bloodletting): In cases of liver-related Ascites, this helps purify the blood.
• Jalaukavacharana (Leech Therapy): Helps in reducing swelling and improving blood circulation.
2. Herbal Treatment (Shamana Chikitsa)
• Punarnava (Boerhavia diffusa): Acts as a natural diuretic, reducing fluid retention.
• Gokshura (Tribulus terrestris): Supports kidney function and reduces swelling.
• Kutki (Picrorhiza kurroa): Improves liver function and digestion.
• Triphala: Detoxifies the digestive tract and prevents Ama accumulation.
• Guduchi (Tinospora cordifolia): Enhances immunity and liver detoxification.
• Sharpunkha (Tephrosia purpurea): Beneficial for cirrhosis-induced Ascites.
3. Diet and Lifestyle (Aahara-Vihara)
• Avoid:
• Salty, spicy, fried, and processed foods.
• Alcohol and excessive protein intake.
• Heavy-to-digest foods like dairy, non-vegetarian meals, and legumes.
• Recommended:
• Light, warm, and easily digestible foods (Moong dal, lauki, barley, buttermilk).
• Coconut water, lemon water, and herbal teas to maintain electrolyte balance.
• Small frequent meals to avoid overloading the digestive system.
4. External Ayurvedic Remedies (Lepa and Herbal Poultices)
• Castor Oil Pack: Applied over the abdomen to reduce fluid accumulation.
• Turmeric and Neem Paste: Helps prevent infection and inflammation.
• Warm Medicated Oil Massage (Abhyanga): Improves lymphatic drainage and circulation.
Conclusion
Ayurveda provides a holistic and long-term approach to treating Ascites by addressing the root cause rather than just removing fluid. With herbal medicines, detoxification therapies, dietary modifications, and lifestyle changes, it strengthens liver, kidney, and digestive function, preventing recurrence and complications.
How Ayurveda is helpful in treating Acne from the Root Cause ?
- March 4, 2025
- Posted by Dr. Vaidya Karanvir Singh
- 0 Comment(s)
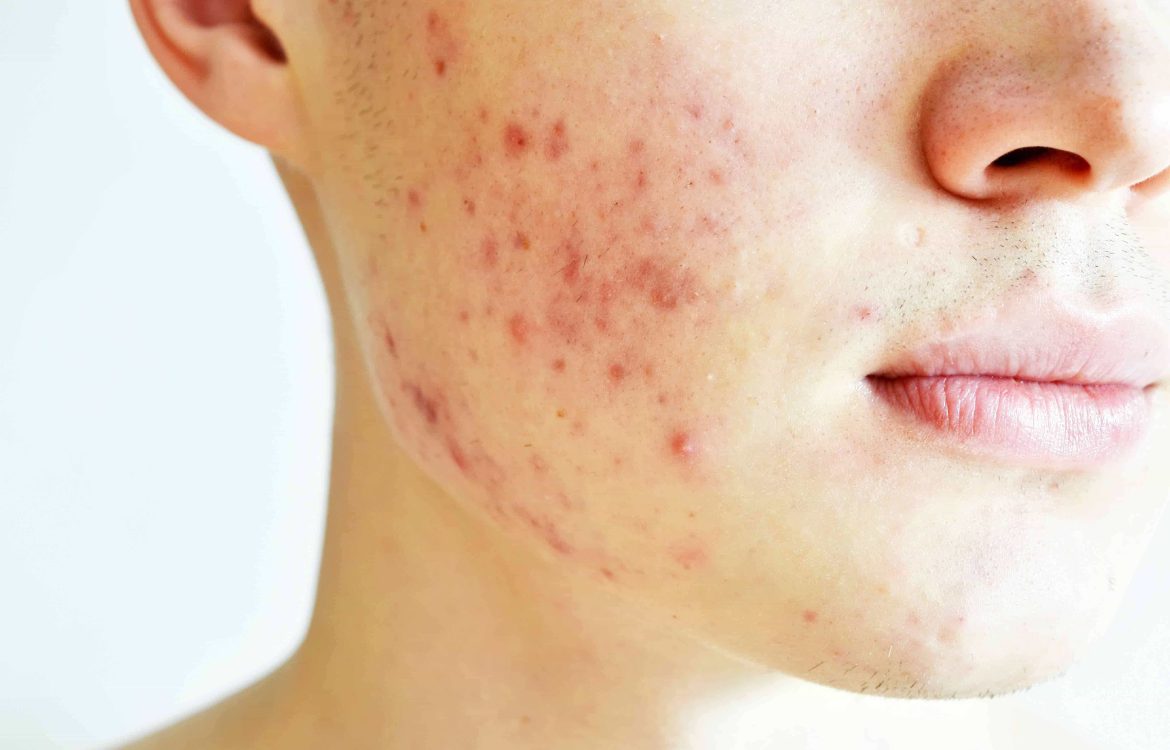
Ayurveda considers acne (Yuvan Pidika) as a Pitta-Vata imbalance, often aggravated by Kapha, leading to excessive heat, toxin accumulation (Ama), and improper digestion. It primarily occurs due to:
• Imbalanced Agni (Digestive Fire) – Weak digestion leads to toxin accumulation.
• Vitiated Rakta (Blood) and Meda Dhatu (Fat Tissue) – Impure blood contributes to acne breakouts.
• Hormonal Imbalance – Seen in aggravated Pitta conditions.
• Excessive Oil and Clogged Pores – Kapha dominance leads to excessive sebum production.
Types of Acne in Modern Science
Modern medicine classifies acne into different types based on severity and symptoms:
1. Comedonal Acne – Blackheads and whiteheads due to clogged pores.
2. Papular Acne – Red, inflamed pimples.
3. Pustular Acne – Pus-filled pimples due to bacterial infection.
4. Nodular Acne – Deep, painful lumps under the skin.
5. Cystic Acne – Large, painful cysts, often causing scars.
6. Hormonal Acne – Caused by fluctuations in hormones.
Difference Between Ayurvedic and Modern Management of Acne
Aspect Ayurveda Modern Medicine
Approach Focuses on root cause healing, balancing Doshas, and detoxification. Treats symptoms using antibiotics, retinoids, and topical treatments.
Treatment Focus Detoxifies the body, corrects digestion, purifies blood, and balances hormones naturally. Uses medications like antibiotics, isotretinoin, and hormonal therapy.
Use of Chemicals Uses herbs, diet, and Panchakarma without side effects. Involves chemical-based treatments that may have side effects like dryness, irritation, or gut issues.
Long-Term Benefits Provides holistic healing and prevents recurrence. Relieves symptoms but may not address the underlying cause, leading to relapse.
Common Ayurvedic Protocol for Acne (Healing from Root Cause)
1. Internal Detoxification (Shodhana Therapy)
• Panchakarma Therapies:
• Virechana (Purgation Therapy): Cleanses excess Pitta and toxins from the liver.
• Raktamokshana (Bloodletting): Removes impure blood in severe cases.
• Nasya (Nasal Therapy): Clears toxins and improves hormonal balance.
2. Herbal Treatment (Shamana Chikitsa)
• Neem (Azadirachta indica): Purifies blood and reduces inflammation.
• Manjistha (Rubia cordifolia): Acts as a natural detoxifier for healthy skin.
• Khadira (Acacia catechu): Excellent for bacterial acne.
• Aloe Vera (Kumari): Soothes and heals acne scars.
• Triphala: Improves digestion and detoxifies the gut, preventing acne.
3. Diet and Lifestyle (Aahara-Vihara)
• Avoid:
• Spicy, oily, junk foods, dairy, and excessive sugar.
• Late-night eating and irregular meal timings.
• Recommended:
• Cooling foods like coconut water, buttermilk, seasonal fruits, and vegetables.
• Herbal teas like coriander, fennel, and mint.
• Drink warm water to improve digestion and toxin removal.
4. External Ayurvedic Remedies (Lepa and Ubtan)
• Neem and Turmeric Paste: Anti-bacterial and anti-inflammatory.
• Multani Mitti (Fuller’s Earth) & Rose Water Mask: Absorbs excess oil.
• Sandalwood & Aloe Vera Gel: Soothes redness and irritation.
Conclusion
Ayurveda not only treats acne but also prevents recurrence by balancing Doshas, detoxifying blood, and correcting digestion. Unlike modern medicine, which focuses on temporary relief, Ayurvedic treatment provides long-term healing without side effects. Combining internal purification, herbal remedies, diet, and lifestyle changes ensures clear, healthy skin from within.
What is the Ayurvedic Approach for Treating Muscle Spasms?
- February 19, 2025
- Posted by Dr. Vaidya Karanvir Singh
- 0 Comment(s)
1. Understanding Muscle Spasms in Modern Science
Muscle spasms (or cramps) are sudden, involuntary muscle contractions that can cause pain and discomfort. They are commonly caused by muscle fatigue, dehydration, nerve compression, or electrolyte imbalances (e.g., low levels of potassium, calcium, or magnesium).
Types of Muscle Spasms in Modern Science:
1. Skeletal Muscle Spasms: Involuntary contractions of voluntary muscles (e.g., legs, back). Often due to overuse, dehydration, or poor circulation.
2. Smooth Muscle Spasms: Affecting internal organs (e.g., stomach cramps or bladder spasms). Often caused by gastrointestinal issues or urinary tract problems.
3. Dystonic Spasms: Neurological in origin, causing muscles to contract abnormally (e.g., writer’s cramp or eyelid twitching).
4. Nocturnal Leg Cramps: Occur during sleep, commonly in the calves or feet.
2. Ayurvedic Perspective on Muscle Spasms (Mamsa-Gata Vata)
In Ayurveda, muscle spasms are linked to an imbalance of Vata dosha, which governs movement, nerve impulses, and muscle function. When Vata becomes aggravated due to poor diet, stress, or injury, it can cause dryness, stiffness, and erratic movements like spasms.
Ayurvedic Causes of Muscle Spasms:
• Vata Vriddhi (Increased Vata) – dryness, irregular lifestyle.
• Poor Rasa Dhatu (Nutritional deficiency).
• Agnimandya (Weak digestive fire) leading to toxin accumulation (Ama).
• Dehydration or lack of Snigdha (moisture) in tissues.
3. Ayurvedic vs. Modern Treatment of Muscle Spasms
Aspect Ayurvedic Approach Modern Medicine
Root Cause Focus Balances doshas, improves digestion, nourishes muscles. Treats symptoms with muscle relaxants or supplements.
Treatment Methods Herbal oils, Panchakarma, dietary corrections. Painkillers, anti-spasmodics, physiotherapy.
Holistic Care Mind-body connection, detoxification, nourishment. Focused on physical symptoms and relief.
Side Effects Minimal with proper diagnosis and treatment. Possible side effects from prolonged medication use.
Long-term Healing Targets underlying imbalances for lasting relief. Symptom management without addressing root cause.
4. Ayurvedic Protocol for Root Cause Healing
A). Shamana (Symptomatic Relief through Herbs)
• Ashwagandha (Withania somnifera): Muscle relaxant, relieves stiffness.
• Nirgundi (Vitex negundo): Anti-inflammatory, reduces nerve pain.
• Bala (Sida cordifolia): Strengthens muscles and nerves.
• Dashmoola: Relieves Vata-related pain and inflammation.
B). Snehana (Oleation Therapy – External and Internal)
• Mahanarayan Taila or Dhanwantharam Taila for external massage to reduce stiffness and improve circulation.
• Internal consumption of medicated ghee like Ksheerabala Taila for chronic Vata imbalance.
C). Swedana (Fomentation Therapy)
• Nadi Sweda (Herbal Steam) or Patra Pinda Sweda (Leaf Bundle Therapy) to relax muscle stiffness.
D). Basti (Medicated Enema Therapy)
• Anuvasana Basti (Oil-based) to lubricate Vata and correct dryness.
• Niruha Basti (Herbal decoction) for chronic conditions.
E). Dietary and Lifestyle Recommendations
• Consume warm, moist, and nourishing foods (e.g., ghee, sesame oil).
• Avoid cold, dry, and processed foods that aggravate Vata.
• Practice gentle yoga (e.g., Pawanmuktasana, Balasana) and meditation.
F). Hydration and Mineral Balance
• Use natural electrolyte sources (e.g., coconut water, rock salt).
• Incorporate calcium- and magnesium-rich foods (e.g., almonds, sesame seeds).
5. Why Ayurveda is More Comprehensive for Muscle Spasms?
• Root Cause Treatment: Ayurveda treats the underlying Vata imbalance and nutritional deficiencies.
• Detoxification: Panchakarma therapies remove toxins (Ama) that disrupt muscle function.
• Holistic Healing: Addresses mind-body balance through diet, lifestyle, and herbal support.
Constipation in Ayurveda vs. Modern Science
- February 19, 2025
- Posted by Dr. Vaidya Karanvir Singh
- 0 Comment(s)
1. Understanding Constipation in Modern Science
In modern medicine, constipation is defined as infrequent bowel movements (fewer than three times a week), difficulty passing stool, or a feeling of incomplete evacuation. It is generally classified into the following types:
• Primary (Functional) Constipation:
• Normal Transit Constipation: Normal movement but difficulty in evacuation due to dietary or lifestyle factors.
• Slow Transit Constipation: Delayed movement through the colon due to reduced motility.
• Pelvic Floor Dysfunction: Poor coordination of pelvic muscles causing difficulty in stool passage.
• Secondary Constipation:
Caused by underlying health conditions (hypothyroidism, diabetes), medications (opioids, antacids), or structural issues (colon obstruction).
2. Ayurvedic Perspective on Constipation (Vibandha)
In Ayurveda, constipation (Vibandha) is primarily associated with an imbalance in Vata dosha—specifically Apana Vayu, which governs the downward movement of waste.
Ayurvedic Causes of Constipation:
• Dry and rough food (Ruksha Ahara)
• Excessive fasting (Langhana)
• Stress and irregular sleeping habits
• Sedentary lifestyle
• Suppressing natural urges (Vega Dharana)
Types of Constipation in Ayurveda:
1. Vataja Vibandha: Dry, hard stools, bloating, pain.
2. Pittaja Vibandha: Burning sensation, yellowish stools, thirst.
3. Kaphaja Vibandha: Sticky stools, heaviness, lethargy.
3. Ayurvedic vs. Modern Treatment of Constipation
Aspect Ayurvedic Approach Modern Management
Root Cause Balancing doshas (mainly Vata) Symptom suppression through laxatives
Treatment Goal Restoring natural bowel movement Immediate relief of constipation
Therapies Panchakarma (e.g., Basti) for detoxification Laxatives, stool softeners, enemas
Long-term Management Dietary and lifestyle changes, herbal support Continuous medication if chronic
Holistic Care Mind-body connection (Stress & Digestion) Focuses mainly on physical symptoms
4. Ayurvedic Protocol for Root Cause Healing
1. Deepan-Pachan (Digestive Fire Activation)
• Use of Hingvastaka Churna to improve digestion.
• Trikatu (Ginger, Black Pepper, Long Pepper) for Ama (toxins) removal.
2. Shodhana (Detoxification through Panchakarma)
• Basti Karma (Medicated Enema) – Best for Vata imbalance and chronic constipation.
3. Shamana (Symptomatic Relief through Herbs)
• Triphala Churna: Mild laxative and colon cleanser.
• Isabgol (Psyllium Husk): Provides fiber for smoother bowel movements.
• Castor Oil (Eranda Taila): Lubricates intestines and promotes elimination.
• Aloe Vera (Kumari Saar): Natural stool softener and intestinal cleanser.
4. Ahara-Vihara (Dietary and Lifestyle Modifications)
• Increase fiber-rich foods (fruits, whole grains, vegetables).
• Warm water with lemon in the morning for bowel stimulation.
• Regular physical activity (e.g., Yoga Asanas like Pawanmuktasana).
5. Stress Management
• Practice meditation and Pranayama (e.g., Anulom-Vilom) to calm Vata.
5. Why Ayurveda is More Comprehensive for Chronic Constipation?
• Root Cause Focus: Treats underlying digestive imbalances rather than masking symptoms.
• Personalized Treatment: Tailored to individual Prakriti (constitution) and dosha imbalances.
• Long-term Healing: Lifestyle adjustments ensure sustainable digestive health.
• Mind-Body Connection: Addresses psychological contributors to constipation.
Would you like a detailed guide on home remedies, Panchakarma steps, or specific herbs?
What is the Ayurvedic Approach to Frozen Shoulder (Apabahuka)?
- February 14, 2025
- Posted by Dr. Vaidya Karanvir Singh
- 0 Comment(s)
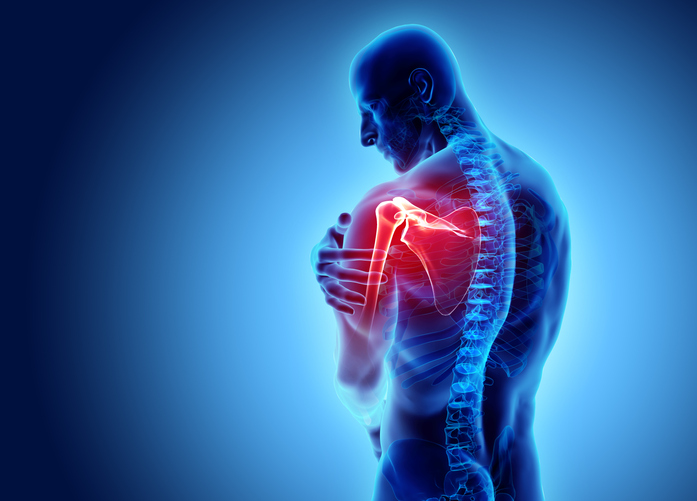
Frozen shoulder, known as Apabahuka in Ayurveda, is a condition characterized by stiffness and pain in the shoulder joint. Ayurveda classifies this disorder primarily as a Vata Vyadhi (a disease caused by aggravated Vata dosha), leading to dryness, stiffness, and restricted movement.
Types of Frozen Shoulder in Modern Science
Modern medicine classifies frozen shoulder into three stages:
1. Freezing Stage (Painful Stage) – Gradual onset of pain and increasing stiffness, lasting from weeks to months.
2. Frozen Stage (Adhesive Stage) – Severe restriction in shoulder movement with persistent stiffness. Pain may decrease but motion remains limited.
3. Thawing Stage (Recovery Stage) – Gradual improvement in mobility as the shoulder heals, but full recovery may take months to years.
Modern medicine attributes frozen shoulder to factors like inflammation, postural issues, diabetes, and trauma, leading to thickening of the shoulder capsule.
Difference Between Ayurvedic and Modern Treatment
Aspect Ayurvedic Treatment Modern Treatment
Approach Root-cause healing by balancing doshas and rejuvenating tissues Symptomatic relief through pain management and physiotherapy
Pain Management Herbs, external therapies like Snehana (oleation), Swedana (sudation), Agnikarma NSAIDs, corticosteroid injections, physiotherapy
Mobility Improvement Panchakarma therapies like Basti, Nasya, Pinda Sweda Physiotherapy, stretching exercises
Long-term Relief Works on reversing Vata imbalance and strengthening muscles Surgery in severe cases
Common Ayurvedic Protocol for Healing the Root Cause
1. Nidana Parivarjana (Removing the Root Cause)
• Avoid cold exposure, sudden heavy lifting, and excessive stress on the shoulders.
• Manage associated conditions like diabetes or cervical spondylosis that may contribute to frozen shoulder.
2. Shodhana Chikitsa (Detoxification & Panchakarma Therapies)
• Snehana (Oleation Therapy): Application of medicated oils like Mahanarayan Taila, Bala Taila to reduce dryness and stiffness.
• Swedana (Fomentation Therapy): Herbal steam therapy to relieve pain and improve flexibility.
• Basti (Medicated Enema): Helps pacify Vata dosha and rejuvenate joints. Oils like Dashmoola or Ksheerbala Taila Basti are beneficial.
• Nasya (Nasal Therapy): Application of Anu Taila or Shadbindu Taila to strengthen nerve function and reduce Vata aggravation.
3. Shamana Chikitsa (Herbal Medicines for Pain & Healing)
• Ashwagandha (Withania somnifera) – Strengthens muscles and relieves pain.
• Guggulu (Commiphora mukul) – Reduces inflammation and improves flexibility.
• Rasna (Pluchea lanceolata) – Effective in relieving joint pain and stiffness.
• Dashmoola – A powerful anti-inflammatory formulation used in decoctions and oils.
• Eranda Taila (Castor Oil) – Acts as a natural pain reliever and Vata pacifier.
4. Agnikarma (Thermal Cauterization Therapy)
• An effective procedure for chronic cases, where controlled heat application reduces stiffness and improves mobility.
5. Diet & Lifestyle Modifications (Pathya-Apathya)
• Include: Warm, oily foods, soups, ghee, milk, nuts, and sesame seeds.
• Avoid: Cold foods, excess dry and raw foods, smoking, and alcohol.
• Exercises: Gentle shoulder rotations, Yoga asanas like Gomukhasana (Cow Face Pose), Bhujangasana (Cobra Pose), Dhanurasana (Bow Pose) to improve flexibility.
Conclusion
Ayurvedic treatment for frozen shoulder focuses on root-cause healing by balancing Vata dosha, improving circulation, and nourishing joints. Unlike modern treatments, which focus primarily on pain relief and physiotherapy, Ayurveda works holistically to restore shoulder mobility, prevent recurrence, and improve overall well-being.
What is the Ayurvedic Perspective and Treatment of GERD?
- February 8, 2025
- Posted by Dr. Vaidya Karanvir Singh
- 0 Comment(s)
Ayurveda approaches gastroesophageal reflux disease (GERD) very differently from modern medicine. Below is an integrated overview covering how Ayurveda views and treats GERD, the modern classification of the condition, and the key differences between Ayurvedic and conventional management.
Ayurvedic Perspective and Treatment of GERD
In Ayurvedic medicine, the symptoms of GERD are often related to an imbalance of the Pitta dosha (which governs heat, acid, and metabolism) and the accumulation of Ama (undigested or “toxic” material) in the gastrointestinal tract. Ayurveda typically does not use the term “GERD” but relates its symptoms to disorders such as Amlapitta (excess acidity or hyperacidity) and Pachakshaya (impaired digestion). The treatment is holistic and individualized, aiming to restore balance by:
• Dietary Modifications:
Ayurveda recommends a cooling, easily digestible diet to reduce excess Pitta. This means avoiding spicy, sour, fried, and processed foods. Instead, one may include foods that are naturally soothing to the stomach (for example, rice gruels, steamed vegetables, and herbal teas).
• Herbal Remedies:
Several herbs are used to balance Pitta and improve Agni (digestive fire). Common remedies include:
• Amla (Indian Gooseberry): Known for its cooling and antioxidant properties, it helps neutralize excess acidity.
• Licorice (Yashtimadhu): Soothes the mucosal lining of the esophagus and stomach, reducing inflammation and irritation.
• Guduchi (Tinospora cordifolia) and Triphala: These support digestion, detoxification, and overall gastrointestinal health.
• Other herbs such as ginger (in small doses) may be used judiciously, as it can stimulate digestion without aggravating acid production when balanced correctly.
• Panchakarma and Lifestyle Changes:
Ayurvedic detoxification therapies (Panchakarma) may be employed to remove Ama and restore the natural functioning of the digestive system. In addition, stress management techniques (such as yoga and meditation) and regular routines (timing of meals, sufficient sleep, and moderate physical activity) are strongly emphasized to maintain overall balance.
Modern Scientific Classification of GERD
In modern gastroenterology, GERD is defined as the reflux of stomach contents into the esophagus that causes troublesome symptoms or complications. Scientific literature generally distinguishes several types or stages of GERD, including:
1. Non-Erosive Reflux Disease (NERD):
Patients experience reflux symptoms without visible esophageal damage on endoscopy.
2. Erosive Esophagitis:
Here, the reflux causes visible inflammation and erosion of the esophageal lining.
3. Barrett’s Esophagus:
This is a complication of chronic reflux where the normal esophageal lining is replaced by columnar epithelium, which can increase the risk of esophageal adenocarcinoma.
4. Functional Heartburn:
A subset where patients have reflux-like symptoms without acid reflux or any mucosal damage.

Modern research also considers factors such as acid exposure time, esophageal motility, and hypersensitivity in the evaluation of GERD.
Differences Between Ayurvedic and Modern Management
• Focus on Root Cause vs. Symptom Relief:
• Modern Management:
Conventional treatment of GERD is largely symptomatic. It typically involves medications such as proton pump inhibitors (PPIs), H2 receptor blockers, and antacids to reduce stomach acid, along with lifestyle modifications (weight loss, dietary changes, avoiding triggers) primarily aimed at reducing symptoms.
Ayurvedic Approach:
Ayurveda seeks to correct the underlying imbalance in the digestive system (especially the Pitta dosha and Ama accumulation). The approach is holistic—it includes a detailed assessment of the individual’s constitution (Prakriti), tailored dietary recommendations, herbal formulations, detoxification therapies, and stress reduction measures to restore overall balance rather than merely suppressing symptoms.
• Customization and Holistic Care:
• Ayurvedic treatments are personalized based on a person’s unique physical and mental makeup. This means that two patients with similar reflux symptoms might receive different herbal formulations, dietary guidelines, and lifestyle advice in Ayurveda.
• Modern medicine, while evidence‐based and standardized in its protocols, often applies a one‐size‐fits‐most strategy for acid suppression.
• Long-Term vs. Short-Term Strategy:
• Modern medications are highly effective in reducing acid secretion in the short term but may not address digestive function or lifestyle factors comprehensively.
• Ayurveda, on the other hand, emphasizes long-term healing through gradual restoration of digestive fire, regular detoxification, and overall lifestyle balance, which proponents believe can lead to sustained improvements in gastrointestinal health.
In Summary
Ayurveda treats GERD by identifying it as an imbalance of digestive energies (mainly an excess of Pitta and accumulation of Ama) and uses a combination of personalized diet, herbal remedies (such as Amla, licorice, Guduchi, and Triphala), detoxification procedures, and lifestyle modifications to restore digestive harmony. In contrast, modern medicine categorizes GERD (including NERD, erosive esophagitis, and Barrett’s esophagus) based on clinical and endoscopic findings and primarily relies on acid suppression and standardized lifestyle changes to manage symptoms.
Both approaches have their merits, and many patients today explore integrative treatments that combine the symptomatic relief of modern medications with the holistic, individualized care offered by Ayurveda. Always consult a healthcare professional before beginning any new treatment plan.
Feel free to ask if you need more detailed information on any aspect of this topic.
Ayurvedic Guide for Vasant Ritu (Spring Season) Diet and Habits
- February 3, 2025
- Posted by Dr. Vaidya Karanvir Singh
- 0 Comment(s)
In Ayurveda, Vasant Ritu (Spring) marks a significant seasonal transition, symbolizing renewal and growth. Occurring between mid-March to mid-May, it is characterized by moderate warmth, blooming flowers, and a rise in humidity. This period naturally increases Kapha dosha, leading to sluggish digestion, respiratory issues, and heaviness in the body. To maintain optimal mental and physical health, Ayurveda recommends adapting diet and lifestyle habits accordingly.
Characteristics of Vasant Ritu
• Moderate temperatures with mild warmth
• Increased Kapha dosha due to melting body fluids accumulated during winter
• Potential for respiratory issues, allergies, indigestion, and lethargy
Dietary Guidelines for Vasant Ritu
1. Light and Dry Foods:
Opt for easily digestible, light meals to counteract Kapha dominance.
• Examples: Barley, millet, roasted grains, and dry vegetables
2. Bitter and Astringent Tastes:
These tastes help pacify Kapha and detoxify the body.
• Examples: Bitter gourd, fenugreek leaves, and neem
3. Spices to Boost Digestion:
Include warming spices to kindle the digestive fire.
• Examples: Ginger, black pepper, turmeric, and cinnamon
4. Seasonal Fruits:
Consume fruits in moderation, avoiding overly sweet varieties.
• Examples: Apples, pomegranates, and pears
5. Limit Heavy and Oily Foods:
Avoid foods that increase Kapha and mucus formation.
• Avoid: Dairy products, fried foods, and excessive sweets
6. Drink Warm Water:
Helps maintain digestion and prevents Kapha buildup.
7. Honey Consumption:
Honey helps dissolve excess Kapha and acts as a natural cleanser.
• How to Use: Mix a teaspoon of honey in warm water daily.
Lifestyle Recommendations for Vasant Ritu
1. Morning Routine (Dinacharya):
• Wake up early (before sunrise)
• Perform tongue scraping and nasya (nasal oil application)
• Practice dry brushing or Udvartana (herbal powder massage) to reduce Kapha
• Take a warm shower
2. Exercise:
Regular physical activity helps reduce Kapha and improves energy levels.
• Recommended Activities: Yoga, brisk walking, and dancing
3. Pranayama (Breathing Exercises):
• Kapalbhati and Anulom Vilom help clear respiratory pathways and balance doshas
4. Sun Exposure:
Spend some time in natural sunlight to counter Kapha heaviness
5. Seasonal Detox (Panchakarma):
• Vamana (therapeutic emesis) is beneficial for Kapha cleansing
6. Clothing:
Wear light and breathable fabrics to stay comfortable
7. Mental Practices:
Engage in meditation and mindfulness to maintain mental clarity and calmness
8. Avoid Daytime Sleep:
Sleeping during the day increases Kapha and causes lethargy
Conclusion
By following these Ayurvedic dietary and lifestyle guidelines during Vasant Ritu, one can achieve a balanced state of mind and body. These practices help detoxify the system, enhance immunity, and promote vibrant energy, setting the foundation for good health throughout the year.
Would you like a detailed meal plan or more information on specific detox practices for this season?